Meropenem
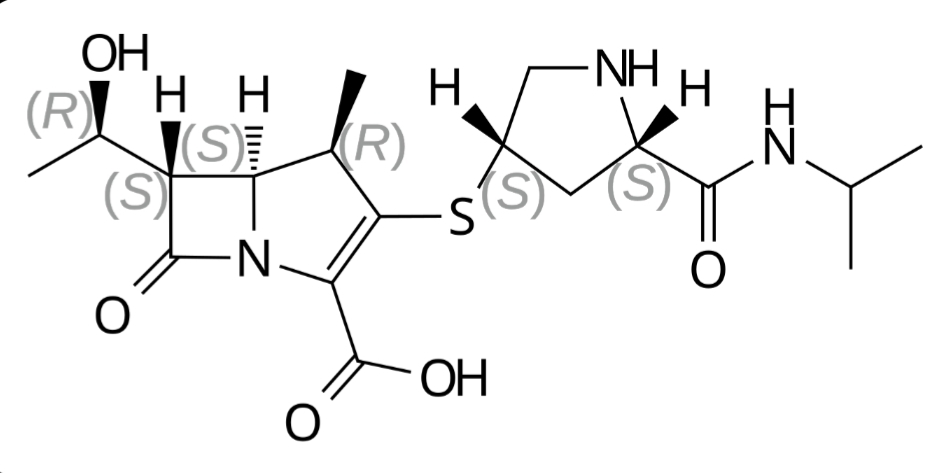
Overview
Meropenem is a broad spectrum carbapenem antibiotic in the beta-lactam class with potent bactericidal activity against many Gram-positive and Gram-negative aerobic and anaerobic bacteria. Its mechanism of action involves inhibition of bacterial cell wall synthesis through binding to penicillin-binding proteins, resulting in bacterial cell death. Meropenem is stable against many beta-lactamases, including extended-spectrum beta-lactamases, although resistance can occur through certain carbapenemase enzymes. It is administered intravenously, usually every eight hours, and is widely used in hospitalized patients for severe or high-risk infections. Meropenem demonstrates good tissue penetration, including into cerebrospinal fluid, which supports its use in central nervous system infections when clinically indicated. Its broad spectrum and predictable pharmacokinetics make it an important option in the management of serious bacterial infections caused by susceptible organisms.
Background and Date of Approval
Meropenem was approved by the United States Food and Drug Administration in 1996 for the treatment of complicated bacterial infections. Following its US approval, it received marketing authorization in the European Union in 1997 for similar indications. Since its initial approval, meropenem has undergone multiple labeling updates and has been approved in numerous countries worldwide. Generic formulations have been approved through abbreviated regulatory pathways over the years, confirming its established role in antimicrobial therapy. Its development and approval were supported by clinical trials demonstrating efficacy in intra-abdominal infections, skin and soft tissue infections, and meningitis.
Uses
Meropenem is indicated for the treatment of complicated skin and skin structure infections, complicated intra-abdominal infections, and bacterial meningitis in pediatric patients aged three months and older. It is also used in severe hospital-acquired infections and other serious infections caused by susceptible Gram-negative and Gram-positive organisms. Meropenem is typically used as monotherapy in infections where broad-spectrum coverage is required, particularly when resistant pathogens are suspected or confirmed. Clinical use should be guided by culture results and local resistance patterns whenever possible.
Administration
Meropenem is administered by intravenous infusion, commonly over 15 to 30 minutes. The standard adult dose for most indications is 1 gram every eight hours. In severe infections such as meningitis, higher doses such as 2 grams every eight hours may be used under specialist supervision. Dosage adjustments are required in patients with renal impairment to reduce the risk of drug accumulation and neurotoxicity. Treatment duration varies depending on infection type and clinical response, typically ranging from seven to 14 days, though longer courses may be required in complicated cases. Monitoring includes clinical assessment and periodic evaluation of renal function.
Side Effects
Common side effects associated with meropenem include nausea, vomiting, diarrhea, headache, rash, and infusion site reactions. Mild and reversible elevations in liver enzymes may occur during therapy. Most adverse reactions are mild to moderate in severity and resolve after completion or discontinuation of treatment. Individual tolerance may vary, and supportive management is generally sufficient.
Warnings
Serious adverse reactions may include hypersensitivity reactions such as anaphylaxis, particularly in patients with a history of allergy to beta-lactam antibiotics. Seizures and other neurologic effects have been reported, especially in patients with renal impairment or pre-existing central nervous system disorders. Clostridioides difficile-associated diarrhea is a recognized risk with broad-spectrum antibiotic use. Meropenem should be avoided in patients with known severe hypersensitivity to carbapenems or related beta-lactam agents, and treatment should be discontinued if severe allergic or neurologic symptoms develop.
Precautions
Assessment of renal function before and during therapy is recommended to guide dosing adjustments. Caution is advised in patients with a history of hypersensitivity to penicillins or cephalosporins due to possible cross-reactivity. Meropenem may reduce plasma concentrations of valproic acid, potentially compromising seizure control, and alternative anticonvulsant therapy may be required. Concomitant administration with nephrotoxic medications necessitates careful monitoring of renal parameters.
Expert Tips
Appropriate use of meropenem should be based on microbiological data and local antimicrobial resistance trends. Renal dose adjustment is critical to optimize therapeutic outcomes and reduce adverse neurologic effects. Patients should be counselled regarding possible gastrointestinal symptoms and advised to report signs of allergic reaction promptly. Integration into antimicrobial stewardship programs supports rational use and helps preserve carbapenem effectiveness against resistant pathogens.
